From the thousands of deaths in Nepal’s capital city Kathmandu and even more ramping up on the plains that border India and the towns and villages and hamlets in the mountains, hospitals and clinics are desperate for oxygen, medicine and vaccines. There is death by COVID-19 and there is death because care-givers cannot access oxygen. With public health care inadequate or non-existent, the pandemic is crushing what is left. Politics are feeding the fire. For the second time in five months, Nepal’s government was dissolved on May 22nd, furthering bureaucratic paralysis. Nepal risks becoming an imploding catastrophe. It is already losing gains it has made in the past years in fighting malnutrition, child labor, early marriage and women’s rights. But if Nepal is a petri dish of disasters, it is also one of innovation and individual dedication. This pandemic once again is a place where despair is often met by individual and community fortitude. Both in the cities and in the rural areas. Nepal’s diaspora has become a major donor https://www.nepalitimes.com/here-now/nepals-diaspora-comes-to-the-rescue/
Then there are those in the pandemic trenches. Here is the story of two doctors- like many others – who are fighting against huge odds.
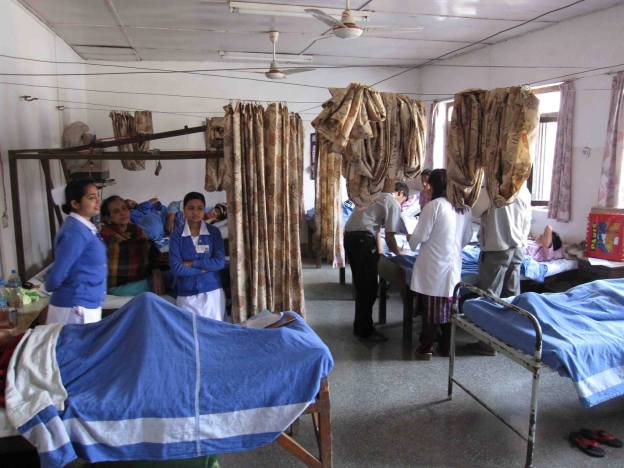
Young medical residents are the backbone of Kathmandu’s COVID wards.

Dr.Prashuma Malla had never felt so helpless. Her patient, a man in his 40s, was suffocating, incapable of drawing in breath. But the hospital ventilators were all occupied and the central supply of oxygen was very low. She pronated her patient while his wife sobbed near him.
“With no oxygen, we can do nothing,” the 28-year-old second year medical resident specializing in anesthesia at Bir Hospital in Kathmandu explained. “It is scary. It is non-stop. I try to tell myself everything is OK. But what can we do?(…)Eight people have died on my watch.”
Malla and her colleagues are on the COVID front lines. Her world is a haze of 36-hour intense and at times terrifying shifts. Bir is Nepal’s oldest and best-known public hospital. As in many Nepali public hospitals, relatives follow patients inside providing food and running to pharmacies to purchase medicine. Bir is overwhelmed. People are sleeping in hallways, stairways, curled up on patients’ beds, pacing from room to room. Doctors believe many relatives are sick as well. The hospital does not have enough PPEs (personal protection equipment). There is a serious shortage of oxygen.
“We are highly exposed,” Malla said of her shifts with the sickest of patients. “Everywhere you go is a COVID ward.” Malla and her colleagues have also become counselors. But with every patient, her job gets harder. Most of the patients are in their 30s and 40s and even many in their 20s. In the chaos, it calms her to explain every detail to relatives. What does it mean to be intubated? Once intubated it is hard to take patients off? Often the patient dies when you extubate. No, they cannot take the body to be cremated. Only police or soldiers can remove it from the hospital.
“They are confused,” she said. “they have never seen someone come off an intubator. I remind them: there is no guarantee.”
Every move Malla and her colleagues make, every decision she takes, she reports to her superior, one of the 3rd year medical residents. And every day at the shift handover, the 3rd year medical students remind Malla about the importance of safety precautions.
At the end of her 36-hour shift, Malla heads home on her moped. The gargantuan traffic in Kathmandu is light because of lockdown. She lives in a tiny two-room apartment with her two brothers. She is terrified of infecting them. She washes immediately including her mask and face shield. Masks always on, they cook together. Briefly unmasked, she eats alone on a miniature terrace. She talks on Viber with her parents in central Nepal. Every day, sometimes every hour, they remind each other to stay safe. She tries to focus on her online medical classes. She doesn’t want to fall behind. But always that nagging fear. Death is there. Near her. Floating and invisible.
***********************************************************************
In Rural Nepal, where a country-wide lockdown and overflowing hospitals are keeping sick people home – ground-breaking telehealth is transforming medical care.
Dr. Hari Neupani is fighting COVID-19 with his cell phone. He leads a team of seven doctors in Dang District, in mid-western Nepal, a land of rural municipalities which shares a border with India and also stretches into Nepal’s mid-range mountains. It is soon rice planting season but a national lockdown has left fields, streets and roads empty, void of the everyday crowds and cacophony of passing trucks.

Telemedicine is new to Nepal. Neupani, who is simultaneously doctor, nurse and mental health expert, is part of Health Foundation Nepal, a Kathmandu-based 501c volunteer-staffed telemedical service that reaches out to patients across 35 districts in Nepal via its Kathmandu hotline. The medical teams are supervised by Dr. Ashok Devkota, a doctor of internal medicine in Providence Rhode Island. The organization’s seven full-time workers and 50 part-time physicians are all volunteers.
Hospitals across Nepal are overflowing. Most of Neupani’s patients have COVID symptoms. Working closely with local governments and hospitals, Neupani’s team identify symptoms, using cell phones – voice, photos and videos – as medical communicators. They connect patients via cell phone with pharmacies and if necessary portable oxygen. The very sick are taken to hospital. So far, the government has acknowledged more than 11,100 cases but doctors believe they are vastly undercounted.
“We focus on people in home isolation and counsel them on the medicines they need and how to get them. We prescribe steroids and do follow-ups and notify local government officials.”
In Dang, where more than 20,000 people live in rural municipalities and villages are isolated, some reachable only on foot, cell phones have become transformative lifelines at many levels. They are a critical means of money transfers from relatives working abroad mostly in menial jobs. These jobs pay school fees, medical bills and even food when the harvest fails. Most recently, the pandemic lock-down has made day-long walks to access medical care, virtually impossible. Even if they could get to a hospital chances of a bed are slim. In Dang there are only 155 intensive care beds and 15 ventilators.

Health Foundation Nepal’s doctors monitor calls in 35 districts across Nepal. With government help, they advertise with local media and newspapers. “This is totally new to Nepal,” Devkota said. “Before COVID it was difficult for people to accept it. But now it will be groundbreaking as we move forward.”
Across Nepal, people are sick on a massive scale. Telehealth cannot take blood tests but has been able to reach hundreds and soon thousands of patients who do not live in urban areas. As long as Neupani’s cell phone stays charged, he is on duty.